3RD BEACH Course - Session 3
Sedation and analgesia during ECMO (M Raes)
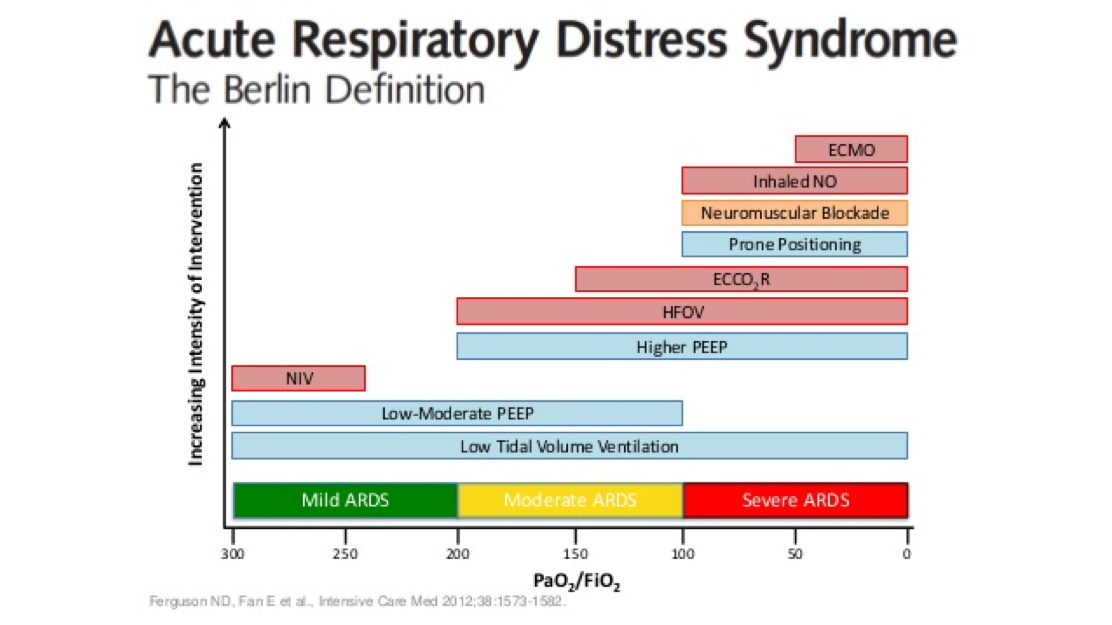
ELSO guidelines suggest moderate to heavy sedation in the first 24 hours
Medicating patients during extracorporeal membrane oxygenation: the evidence is building
Volatile sedation in the intensive care unit A systematic review and meta-analysis
Inhalative sedation with small tidal volumes under venovenous ECMO.
CONCLUSION
- Do we need to sedate our ECMO patient?
- Not all patients
- Perhaps ‘less’ is ‘more’
- Major clinical challenge (especially in VV-ECMO)
- Scarce data
- What is the best sedation strategy?
- No consensus
- Sequestration on ECMO needs higher doses in most drugs
- Inhaled anesthetics promising alternative?
- Should we monitor?
- YES!
Weaning from ECMO (D dos Reis Miranda)
VV-ECMO
When to do wean trial?
- FiO2 < 60%
- Vt 4-6 ml/kg
- Driving pressure < 15 mbar
- PEEP < 15 mbar
VA-ECMO
Decrease blood flow
-
Approx. 1 l/min for LV failure
-
Approx. 0.5 l/min for RV failure
CONCLUSION
VV ECMO
- Do not decrease ECMO blood flow
- Set ECMO gasflow off at reasonable vent setting
- Maintain this for couple of hours (practical: overnight)
VA ECMO
- Do not decrease ECMO gasflow
- Set reasonable vent setting
- Decrease ECMObloodflow to 0.5 - 1.0 liter/min for 5-15 min
- Do not solely rely on macrohemodynamic parameters
- Use echo or microcirculation