IFAD Day 2
IFAD2015 Day 2 Blog summary
PLENARY SESSION (Chairs: A. Perel - D. Lobo)
Opening Lecture: Perioperative fluids - How restrictive should we go? (M. Mythen)
Distinct from the critical care situation
Guiding fluid therapy - Knowledge and experience vs advanced haemodynamic monitoring
BJA 2015 Lilot – dependent on anaesthesia provider. Huge variation in amount given (http://bja.oxfordjournals.org/content/early/2015/01/13/bja.aeu452)
It’s not the water that does the harm, it’s the SALT
Is it the restriction of fluid or the avoidance of overload that is of benefit?
http://www.ncbi.nlm.nih.gov/pubmed/22253274 - meta-analysis
Perioperative Fluid Utilization Variability and Association With Outcomes - http://journals.lww.com/annalsofsurgery/Abstract/publishahead/Perioperative_Fluid_Utilization_Variability_and.97236.aspx
The definition of liberal and restrictive fluid strategies are very different between the studies
REstrictive Versus LIbEral Fluid Therapy in Major Abdominal Surgery: RELIEF Study -
https://clinicaltrials.gov/ct2/show/NCT01424150
Perioperative fluid management: Consensus statement from the enhanced recovery partnership - http://perioperativemedicinejournal.biomedcentral.com/articles/10.1186/2047-0525-1-2
PRO-CON Debate: Blood Transfusion on the ICU
CON: Don't exaggerate! (A. Perner)
Transfusion issues – expensive and limited resource, known side-effects, benefits vs harm
Risk of anaemia – low DO2, ischaemia, organ dysfunction
Risk of transfusion – infectious and non-infectious
Cochrane review - http://www.ncbi.nlm.nih.gov/pubmed/22513904
TRISS trial - http://www.nejm.org/doi/full/10.1056/NEJMoa1406617
TITRE2 trial - http://www.nejm.org/doi/full/10.1056/NEJMoa1403612
Association of Blood Transfusion With Increased Mortality in Myocardial Infarction
A Meta-analysis and Diversity-Adjusted Study Sequential Analysis - http://archinte.jamanetwork.com/article.aspx?articleid=1485987
PRO: Don't hold back! (C. Ince)
Blood transfusions are the only effective therapy to improve oxygen delivery
The original TRICC trial - http://www.nejm.org/doi/full/10.1056/NEJM199902113400601
Problem with trials - absence of evidence is not evidence of absence
Single centre trials are better than multicenter trials?
PRO-CON Debate: Blood Transfusion on the ICU
CON: Don't exaggerate! (A. Perner)
Transfusion issues – expensive and limited resource, known side-effects, benefits vs harm
Risk of anaemia – low DO2, ischaemia, organ dysfunction
Risk of transfusion – infectious and non-infectious
Cochrane review - http://www.ncbi.nlm.nih.gov/pubmed/22513904
TRISS trial - http://www.nejm.org/doi/full/10.1056/NEJMoa1406617
TITRE2 trial - http://www.nejm.org/doi/full/10.1056/NEJMoa1403612
Association of Blood Transfusion With Increased Mortality in Myocardial Infarction
A Meta-analysis and Diversity-Adjusted Study Sequential Analysis - http://archinte.jamanetwork.com/article.aspx?articleid=1485987
PRO: Don't hold back! (C. Ince)
Blood transfusions are the only effective therapy to improve oxygen delivery
The original TRICC trial - http://www.nejm.org/doi/full/10.1056/NEJM199902113400601
Problem with trials - absence of evidence is not evidence of absence
Single centre trials are better than multicenter trials?
ARDS & SEPSIS (Chairs: A. Wilmer - Ph. Jorens)
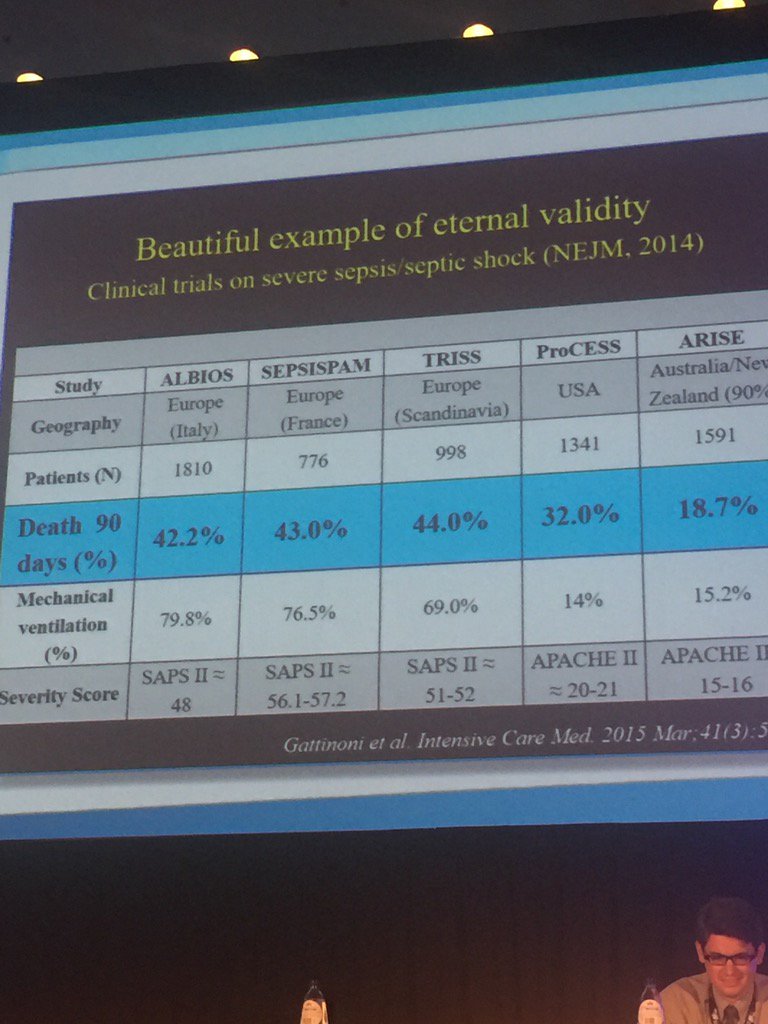
What everyone should know about treating ARDS! (L. Gattinoni)
Lung protective strategy = less energy + more homogeneous lung
Recipe
- Assess Severity
- Select Tidal Volume
- Select PEEP
- Select RR-IE
- Watch haemodynamics
Severity = P/F ratio at 5cmH2O PEEP (300 200 100 Berlin definition)
Tidal volume = 6mls/kg IBW (check plateau pressure)
PEEP = based on gas exchange http://www.ncbi.nlm.nih.gov/pubmed/24196193
- Mild ARDS <10cmH2O
- Mod ARDS 10-15 cmH2O
- Severe ARDS > 15cmH2O
PRO-CON Debate: ARDS
The monitored approach: D. Reuter
Individualised care – understand pathophysiology à determined individual therapy
Fluid therapy in ARDS - http://journal.publications.chestnet.org/article.aspx?articleid=1089902
Assessing Extracellular Lung Water Index is difficult (Clinical vs Monitors)
- Clinically - http://www.ncbi.nlm.nih.gov/pubmed/21273034
- Ultrasound - http://www.atsjournals.org/doi/abs/10.1164/ajrccm.156.5.96-07096#.VlmBU4RH2Rs
The clinical approach: JL. Vincent
Do we need ARDS? - http://link.springer.com/article/10.1007%2Fs00134-015-4120-7
Avoid fluid overload! Which patients will benefit from fluids (pic)
Patients die with ARDS not because of ARDS
What's left of GDT in sepsis? (A. Perel)
10 Short Beliefs in ICM - http://link.springer.com/article/10.1007/s00134-015-3733-1
Bench-to-bedside review: the initial hemodynamic resuscitation of the septic patient according to Surviving Sepsis Campaign guidelines--does one size fit all? - http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2592726/
The Surviving Sepsis Campaign bundles and outcome: results from the International Multicentre Prevalence Study on Sepsis (the IMPreSS study) - http://link.springer.com/article/10.1007%2Fs00134-015-3906-y
Management of septic shock: a protocol-less approach - http://www.ncbi.nlm.nih.gov/pubmed/26088759
Treating septic shock responsibly

PERIOPERATIVE FLUID MANAGEMENT (Chairs: D. Lobo - M.Mythen)
BEFORE SURGERY: Do we need prophylactic colloids? (R. Hahn)
Rationale - Pre-loading prevents undetected hypovolaemia
Interactions between the volume effects of hydroxyethyl starch 130/0.4 and Ringer´s acetate -http://www.ccforum.com/content/17/3/R104
No role for prophylactic colloid
Crystalloids fluids have better plasma volume expanding properties
Colloids should only be given on special indications only
DURING SURGERY : Fluid choices in the Elderly (D. Lobo)
AAGBI Guidelines Peri-operative Care of the Elderly 2014
https://www.aagbi.org/sites/default/files/perioperative_care_of_the_elderly_2014.pdf
WTOTW - http://www.anaesthesiauk.com/documents/elderly.pdf
Fluids and GI function - http://www.ncbi.nlm.nih.gov/pubmed/21681086
AFTER SURGERY: Colloids vs Crystalloids in Postop Shock (D. Annane)
SAFE study - http://www.nejm.org/doi/pdf/10.1056/nejmoa040232
CHEST study - http://www.nejm.org/doi/full/10.1056/NEJMoa1209759
CRISTAL study - http://jama.jamanetwork.com/article.aspx?articleid=1752245
AFTER SURGERY: Enhancing surgical recovery (M. Mythen)
Royal College of Anaesthetist UK film on perioperative medicine - http://www.rcoa.ac.uk/periopmed/animation
Why is the high-risk surgical patient still at risk? http://bja.oxfordjournals.org/content/106/3/289.full.pdf+html
Enhancing Recovery Pathway patients are eating, drinking and mobilizing within 24 hours
Pillars or ERS – minimally invasive surgery, manage pain and fluids
Enhanced recovery from surgery in the UK: an audit of the enhanced recovery partnership programme 2009–2012 -http://bja.oxfordjournals.org/content/115/4/560.long
FLUID OVERLOAD (Chairs: A. Wilmer - D. Annane)
Is hypervolemia really so bad? In the operating room (R. Hahn)
Risk of hypervolaemia leads to increased risk of pulmonary oedema and increased secretion of ANP (increase protein extravasation and causes albuminuria)
Hypervolemia increases release of atrial natriuretic peptide and shedding of the endothelial glycocalyx -http://www.ccforum.com/content/18/5/538
Must hypervolaemia be avoided? https://www.google.be/url?sa=t&rct=j&q=&esrc=s&source=web&cd=2&ved=0ahUKEwjt8KKErrPJAhVBKg4KHQlvBKsQFggsMAE&url=https%3A%2F%2Fjournals.viamedica.pl%2Fanestezjologia_intensywnaterapia%2Farticle%2Fdownload%2FAIT.a2015.0062%2F29991&usg=AFQjCNEiJqdG5oRsn1t75G0qH9rddUacsA
Is hypervolemia really so bad? In the ICU (JL. Vincent)
The adverse effect (if any) of the hypervolaemic state on ICU is dependent on the time course of the patient’s illness
Higher vs. lower fluid volume for septic shock: clinical characteristics and outcome in unselected patients in a prospective, multicenter cohort -http://www.ccforum.com/content/16/3/R76
SOSD approach – Salvage Optimisation Stabilisation De-escalation
4 phases of IV fluid therapy - http://bja.oxfordjournals.org/content/113/5/740.abstract
Sepsis in European intensive care units: results of the SOAP study - http://www.ncbi.nlm.nih.gov/pubmed/16424713
FINAKKI study - http://www.ccforum.com/content/16/5/R197
Furosemide 5mg as a test to see if a patient is ready for de-escalation is advocated by Prof Vincent and Dr Perel
Is de-resuscitation the solution? (I. De laet)
Fluid overload in patients with severe sepsis and septic shock treated with early goal-directed therapy is associated with increased acute need for fluid-related medical interventions and hospital death - http://www.ncbi.nlm.nih.gov/pubmed/25247784
How to avoid fluid overload -http://www.ncbi.nlm.nih.gov/pubmed/26103147
Fluid overload, de-resuscitation, and outcomes in critically ill or injured patients: a systematic review with suggestions for clinical practice - http://www.ncbi.nlm.nih.gov/pubmed/25432556
How to de-resuscitate? Furosemide or ultrafiltration.
Ensure absence of shock or tissue hypoperfusion
- Define clinical endpoint
- Set fluid balance goal
- Set perfusion and renal safety precautions
- Re-evaluate after 24 hours
- Adjust plan accordingly
CLOSING SESSION (Chairs: D. Himpe - P. Elbers)
Non-invasive monitoring of oxygen delivery: new frontiers (A. Perel)
- ORI oxygen reserve index – non invasive and continuous device made by Masimo
- Continuous non-invasive Hb monitoring
- Pleth variation index
Standardization of care: impact of an enhanced recovery protocol on length of stay, complications, and direct costs after colorectal surgery -http://www.ncbi.nlm.nih.gov/pubmed/25797725
Pleth variability index is a weak predictor of fluid responsiveness in patients receiving norepinephrine -http://www.ncbi.nlm.nih.gov/pubmed/23103777
Non-invasive monitoring of oxygen delivery in acutely ill patients: new frontiers -
http://www.annalsofintensivecare.com/content/pdf/s13613-015-0067-7.pdf
Intensive Care Anno 2015 - What can we do better? (L. Gattinoni)
Extracorporeal Membrane Oxygenation in Severe Acute Respiratory Failure A Randomized Prospective Study - http://jama.jamanetwork.com/article.aspx?articleid=367396
Gattinoni – ICM (pic)